
metmike: I had COVID in early August and will wait until November to get this shot.
Good Data sources:
https://coronavirus.1point3acres.com/en
COVID Data Tracker
https://covid.cdc.gov/covid-data-tracker/#vaccinations_vacc-people-additional-dose-totalpop
https://ourworldindata.org/coronavirus/country/united-states

Previous threads on COVID with some good links:
COVID 4-2-22
Started by metmike - Jan. 1, 2022, 4:26 p.m.
https://www.marketforum.com/forum/topic/79750/
Statistics on COVID/opinions +Virus Season/Weather
Started by metmike - Nov. 11, 2021, 7:54 p.m.
https://www.marketforum.com/forum/topic/77622/
Will we have a COVID season this Winter?
Odds/science greatly favors it. I spent a great deal of time researching the studies/empirical data/evidence about this and will share some of it again:
Virus's love dry air. In the numerous scientific studies on virus's done before COVID, what they found was, when they doubled the ABSOLUTE humidity in the laboratory, the amount of virus that was able to survive after one hour was cut by 50%.
Conversely, when you DECREASE the absolute humidity by 50%, the amount of virus that survives after 1 hour is doubled.
This is a huge contribution/reason for virus's to increase in the Winter.
https://www.cdc.gov/flu/about/season/flu-season.htm
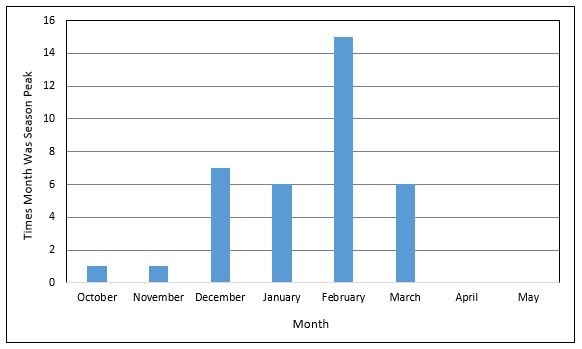
An illustrated explanation of why the world's most obnoxious virus at least doesn't stick around all year.
https://www.popsci.com/science/article/2013-01/fyi-why-winter-flu-season/
Palese decided to test theory #3–the idea that the flu virus does better in cold, dry air than warm, humid air. He acquired some guinea pigs and ran several experiments to see how temperature and humidity affect the way the flu spreads. In each experiment, he injected half the guinea pigs with influenza A (the common flu), and put them in a crate next to a crate of uninfected animals.
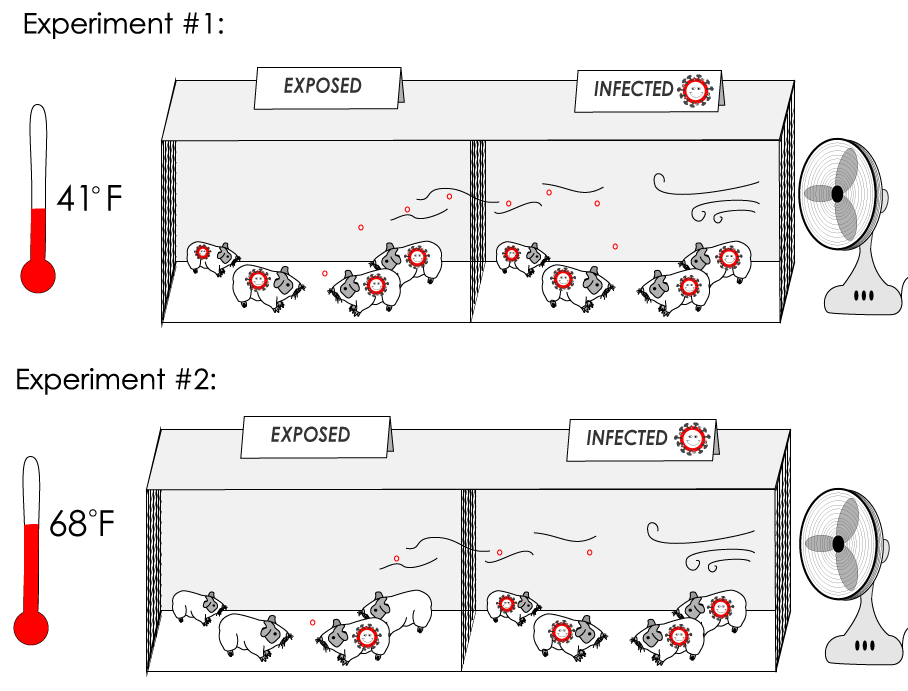
Guinea Pig Experiment
At a temperature of 41 degrees(low absolute humidity), all four of the exposed guinea pigs caught the flu, but when Palese repeated the experiment at 68 degrees, only one of the exposed animals was infected. And when he and his colleagues ran the test at a temperature of 86 degrees, none of the exposed animals got sick.
Several studies have made the case for this “transmission” hypothesis since Palese’s guinea pig study, but other researchers think the biggest factor is actually the virus’s survival. One study found that the flu virus survives for much longer in low humidity than high humidity:

https://papers.ssrn.com/sol3/Papers.cfm?abstract_id=3551767
Using the daily R values from January 21 to 23, 2020 as proxies of non-intervened transmission intensity, we find, under a linear regression framework for 100 Chinese cities, high temperature and high relative humidity significantly reduce the transmission of COVID-19, respectively, even after controlling for population density and GDP per capita of cities. One degree Celsius increase in temperature and one percent increase in relative humidity lower R by 0.0383 and 0.0224, respectively. This result is consistent with the fact that the high temperature and high humidity significantly reduce the transmission of influenza. It indicates that the arrival of summer and rainy season in the northern hemisphere can effectively reduce the transmission of the COVID-19.
file:///C:/Users/Basement/Downloads/SSRN-id3551767(1).pdf
Using the value R to represent the transmission, the paper also found that cities in northern China, where temperatures and relative humidity were lower, had larger transmission values than cities along the country's southeast coast.

The scientists' findings align with what some experts have suspected about weather's impact, including Hong Kong University pathology professor John Nicholls, who told AccuWeather that research on a lab-grown copy of SARS-CoV-2, "in cold environments, there is longer virus survival than warm ones."
Total virus collected for 60 minutes retained 70.6–77.3% infectivity at relative humidity ≤23% but only 14.6–22.2% at relative humidity ≥43%. Analysis of the individual aerosol fractions showed a similar loss in infectivity among the fractions. Time interval analysis showed that most of the loss in infectivity within each aerosol fraction occurred 0–15 minutes after coughing. Thereafter, losses in infectivity continued up to 5 hours after coughing, however, the rate of decline at 45% relative humidity was not statistically different than that at 20% regardless of the aerosol fraction analyzed.
At low relative humidity, influenza retains maximal infectivity and inactivation of the virus at higher relative humidity occurs rapidly after coughing. Although virus carried on aerosol particles <4 µM have the potential for remaining suspended in air currents longer and traveling further distances than those on larger particles, their rapid inactivation at high humidity tempers this concern. Maintaining indoor relative humidity >40% will significantly reduce the infectivity of aerosolized virus
Washington, D.C., March 13, 2020 (GLOBE NEWSWIRE) -- What can the public do to defend against the COVID-19 coronavirus? One simple answer is to ramp up humidification at home and in the workplace, if humidity levels are low. Hospitals treating cases of viral respiratory infection may be advised to do the same.
Why has the novel coronavirus COVID-19 had only a minimal impact in tropical countries while temperate zone countries such as China, Korea, Italy, Iran and the United States have suffered outbreaks? Humidity, and especially indoor humidity, seems to hold the key.
++++++++++++++++++++++++++++++++++++++++++
https://www.sciencedaily.com/releases/2019/05/190513155635.htm
While experts know that cold temperatures and low humidity promote transmission of the flu virus, less is understood about the effect of decreased humidity on the immune system's defenses against flu infection.
++++++++++++++++++++++++++++
https://www.bbc.com/future/article/20151016-the-real-reason-germs-spread-in-the-winter
+++++++++++++++++
Lab experiments, for instance, have looked at the way flu spreads among groups of guinea pigs. In moister air, the epidemic struggles to build momentum, whereas in drier conditions it spreads like wildfire. And comparing 30 years’ worth of climate records with health records, Jeffrey Shaman at Columbia University and colleagues found that flu epidemics almost always followed a drop in air humidity.
In fact, the overlap of the graphs was so close, “you could pretty much put one on top of each other,” says Metz, who together with Adam Finn, recently reviewed all the evidence for the Journal of Infection. The finding has now been replicated many times including analyses of the 2009 Swine flu pandemic.
https://journals.plos.org/plosbiology/article?id=10.1371/journal.pbio.1000316
Much of the observed wintertime increase of mortality in temperate regions is attributed to seasonal influenza. A recent reanalysis of laboratory experiments indicates that absolute humidity strongly modulates the airborne survival and transmission of the influenza virus. Here, we extend these findings to the human population level, showing that the onset of increased wintertime influenza-related mortality in the United States is associated with anomalously low absolute humidity levels during the prior weeks. We then use an epidemiological model, in which observed absolute humidity conditions temper influenza transmission rates, to successfully simulate the seasonal cycle of observed influenza-related mortality. The model results indicate that direct modulation of influenza transmissibility by absolute humidity alone is sufficient to produce this observed seasonality. These findings provide epidemiological support for the hypothesis that absolute humidity drives seasonal variations of influenza transmission in temperate regions.
++++++++++++++++++++++++++++++
https://jvi.asm.org/content/88/14/7692.short
https://jvi.asm.org/content/jvi/88/14/7692.full.pdf
+++++++++++++++++++++++++++++++
https://bmcinfectdis.biomedcentral.com/articles/10.1186/1471-2334-13-71
Low absolute humidity (AH) has been associated with increased influenza virus survival and transmissibility and the onset of seasonal influenza outbreaks. Humidification of indoor environments may mitigate viral transmission and may be an important control strategy, particularly in schools where viral transmission is common and contributes to the spread of influenza in communities.

https://aem.asm.org/content/76/12/3943.full
+++++++++++++++++++
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2034399/
In temperate regions influenza epidemics recur with marked seasonality: in the northern hemisphere the influenza season spans November to March, while in the southern hemisphere epidemics last from May until September. Although seasonality is one of the most familiar features of influenza, it is also one of the least understood. Indoor crowding during cold weather, seasonal fluctuations in host immune responses, and environmental factors, including relative humidity, temperature, and UV radiation have all been suggested to account for this phenomenon, but none of these hypotheses has been tested directly. Using the guinea pig model, we have evaluated the effects of temperature and relative humidity on influenza virus spread. By housing infected and naïve guinea pigs together in an environmental chamber, we carried out transmission experiments under conditions of controlled temperature and humidity. We found that low relative humidities of 20%–35% were most favorable, while transmission was completely blocked at a high relative humidity of 80%. Furthermore, when guinea pigs were kept at 5 °C, transmission occurred with greater frequency than at 20 °C, while at 30 °C, no transmission was detected. Our data implicate low relative humidities produced by indoor heating and cold temperatures as features of winter that favor influenza virus spread.
++++++++++++++++++++++++++
Low humidity fuels spread of viruses, new research finds
It's one of the hallmarks of winter: The misery of being stuck in bed with the flu. Now, scientists are finally figuring out why the virus hits hardest in the wintertime and why some winters are worse than others.
Extremely low humidity levels in winter, according to new research, fuel influenza outbreaks. Particularly dry spells make the problem worse. The discovery might help scientists prepare for epidemics and for the rash of secondary illnesses, like pneumonia, that often slam people once they're already down.
"It is the first step toward potentially forecasting the risk of influenza outbreaks," said Jeffrey Shaman, an atmospheric scientist at Oregon State University in Corvallis. "By getting a handle on what's going on with influenza, we are also getting a handle on the other diseases that really piggy back on influenza."
To explain why flu and related illnesses strike far more often in the winter than at other times of year, theories have fallen into three categories. One idea is that people spend more time indoors in the winter and schools are in session, so there is more person-to-person contact.
Another theory is that, with less exposure to sunlight, people have lower levels of melatonin and vitamin D, weakening their immune systems and making them more likely to succumb to influenza viruses. Scientists have also hypothesized that temperature and humidity affect how long the virus can last after someone coughs or sneezes.
Previous research has shown that influenza viruses survive longer in air when temperatures are colder and relative humidity is lower. Relative humidity, which appears in many weather reports, describes how close conditions are to the point of forming fog or clouds.
But relative humidity isn't the best measurement for studying flu outbreaks, Shaman said, because relative humidity varies with temperature. So, there is actually less moisture in the air on a rainy winter day in Seattle than there is on a sunny summer day in the same city.
He thought it would be more useful to look at absolute humidity, which measures exactly how much moisture is in the air, regardless of temperature.
On that scale, Shaman said, winters are usually twice as dry as summers in a place like San Diego and Arizona, four times drier in New York, and up to five times drier in a particularly cold state like Minnesota.
Along with colleagues, he analyzed 31 years of data from around the United States and used a computer model to show that influenza outbreaks were more likely to occur when absolute humidity levels were low. Like a sliding scale, progressively drier air led to progressively higher likelihood that an outbreak would occur, the researchers reported in the journal PLoS Biology. Temperature didn't play much of a role.
"People had recognized that there was seasonality to this, but nobody has really come up with a unifying explanation," said Gregory Poland, Director of the Mayo Clinic's Vaccine Research Group in Rochester, Minn. Humidity, he said, "is likely is part of that unifying explanation."
Humidity is probably not the only explanation, however, and the weather forecast will probably never serve as a flu forecast. Even in dry conditions, the virus needs to be hanging around, and people need to come into contact to spread it. Still, any insight into what drives epidemics is a step toward saving lives.
When absolute humidity is low, for example, local hospitals could start stockpiling anti-viral medications and other supplies, and they could increase moisture levels in patient rooms.
https://www.nih.gov/news-events/nih-research-matters/dry-air-may-spur-flu-outbreaks
"In PLoS Biology on February 23, 2010, the researchers reported that there were often significant drops in absolute humidity in the weeks prior to a flu outbreak. "This dry period is not a requirement for triggering an influenza outbreak, but it was present in 55-60% of the outbreaks we analyzed, so it appears to increase the likelihood of an outbreak," Shaman says. "The virus response is almost immediate; transmission and survival rates increase and about 10 days later, the observed influenza mortality rates follow."
This discovery might be used in the future to help predict when outbreaks will occur. It also has implications for treating influenza outbreaks. For example, hospitals may pay more attention to controlling humidity levels.
"Obviously there are tradeoffs because influenza is not the only pathogen out there," Shaman says. "There are pathogenic molds that flourish in higher humidity. But if the immediate concern is an outbreak of influenza, it may be worthwhile to raise humidity levels."
metmike: If this is true of COVID-19, then we should be elevating humidity levels in hospitals to help decrease the survival time by 50% in the drier air. However, considering the protective gear being worn by health care workers already, it may not have that great of an affect.
++++++++++++++++++++++++++++++++++++
https://www.the-sun.com/news/723902/coronavirus-dies-sunlight-us-homeland-security-study/
The game-changing findings of the joint effort between the DHS's Science and Technology directorate and Donald Trump's coronavirus task force was revealed at Thursday's White House press briefing.
The virus dies quickest in the presence of direct sunlight, and it survives best in indoor conditions, the study found.

If wearing a mask............use one that is effective, an N95 mask!
I usually don't wear a mask these days, unless its mandatory at a medical facility.
While cloth masks are better than nothing because they can filter out the larger particles/aerosols that get trapped(and especially help to protect other people from a coughing/sneezing infected person), the N95s filter out 95% of the particles, including the larger AND smaller ones.
Almost everyone is still wearing the cloth masks. I asked my wife and she notices the same thing.
At the very start of the pandemic, they briefly stated that wearing a mask is not recommended. Then, they quickly changed it to telling people to only wear cloth masks so that we could save the N95s for people in the medical profession that need them and wearing the cloth masks for protection has been permanently etched into people brains/habits.
They have done a horrible job in stressing the much more effective N95 masks since supplies were no longer an issue a long time ago.
Wearing N95s instead of cloth masks may have been able to save hundreds of thousands of lives.
Why N95, KN95 masks are so much more effective than cloth
Started by metmike - Jan. 10, 2022, 9:44 p.m.
https://www.marketforum.com/forum/topic/80194/
Get N95 masks ASAP! Here's the truth.
28 responses |
Started by metmike - Dec. 21, 2020, 7:27 p.m.
https://www.marketforum.com/forum/topic/63115/